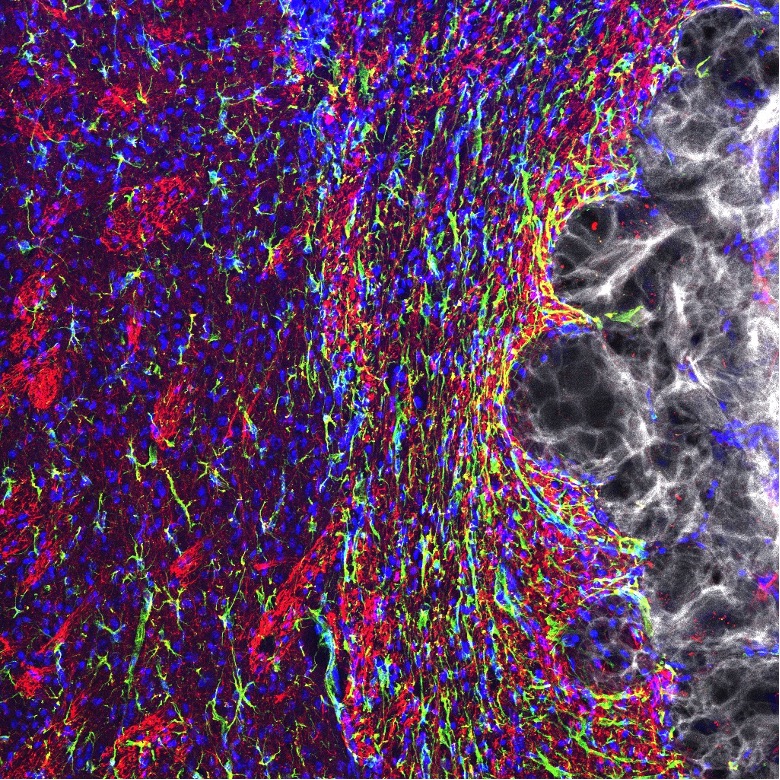
Biomaterial therapy for healing brain tissue after ischemic stroke
Unmet Need
Ischemic stroke affects 692,000 patients annually in the United States, and can result in paralysis and complications related to cognition and motor function. After a stroke, scarring and atrophy can occur at the site of injury in the brain, or the stroke core, preventing the brain from restoring tissue function. Currently, stroke rehabilitation is focused on speech and physical therapy, but there are few therapies that help regenerate neural tissue and prevent atrophy of the brain. Therefore, there is a need for regenerative medicines that directly promote regrowth and healing of brain tissue after a stroke, allowing for functional restoration at the stroke core.
Technology
Duke inventors have developed a biomaterial stroke therapy that promotes the regrowth of brain tissue at the stroke core and prevents scarring and atrophy in the brain. This material is intended to be injected into the stroke core and provide a pro-healing, anti-scarring scaffold for brain tissue and blood vessels to regrow into the injured area. Specifically, this biomaterial is a Micro-Annealed Particle (MAP) gel of peptide-functionalized hyaluronic acid microbeads. These beads are modified with peptides that promote cell adhesion and form a biocompatible, highly porous 3D hydrogel scaffold that promote the ingrowth and functional maturation of neural and vascular cells. This facilitates volumetric restoration of brain tissue and the prevention of inflammation and scar tissue formation. As the cells grow into the scaffold, the gel naturally breaks down over time and is replaced with healthy tissue. This has been demonstrated in a mouse model of ischemic stroke, where the MAP gel promoted ingrowth and pro-healing behavior of astrocytes and microglia, key cellular modulators of neural recovery, as was as revascularization at the stroke core and restoration of brain volume. These results demonstrate the ability of the MAP gel to prevent brain atrophy and scarring associate with ischemic stroke.
Other Applications
This technology could also potentially be used as a therapy for other injuries and pro-inflammatory conditions of the central nervous system where there is damage to brain tissue, such as a traumatic brain injury. Additionally, to augment the pro-healing effects of the hydrogel alone, this technology could be co-administered or used as a carrier for other treatments such as small-molecule drugs, biologics, and cell therapies.
Advantages
- Because this therapy is biomaterial-based, it has fewer concerns with batch-to-batch variability, supply chain cold storage, and patient immune response than biologic- or cell-based regenerative medicine therapies
- Transient therapy that is naturally replaced with healthy tissue over time, as compared to a permanent electrical implant such as a vagal nerve stimulus device
- Proven success in mouse model of stroke, specifically by promoting a pro-healing, anti-scarring response in multiple key neural cell types, vasculature, and at the tissue-level